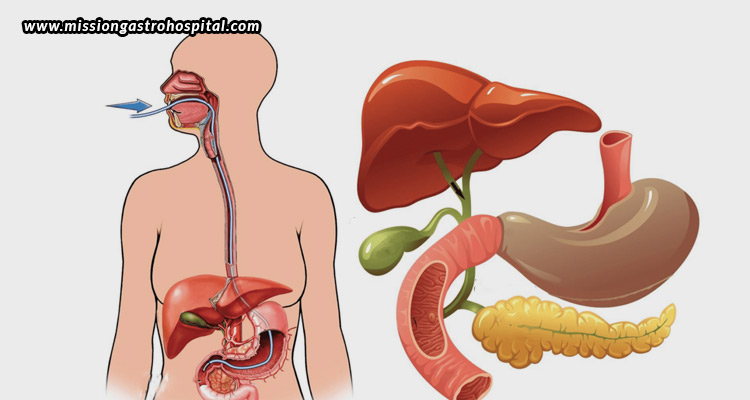
When dealing with intricate issues related to the bile ducts, liver, gallbladder, and pancreas, few procedures offer as much diagnostic and therapeutic precision as ERCP. However, like any medical procedure, ERCP carries certain risks. For patients contemplating this procedure, it is crucial to comprehend both the possible benefits and the related complications to make a well-informed choice – especially in situations where the clinical necessity is pressing or treatment alternatives are scarce. This blog presents a clear, balanced overview of the most prevalent benefits and risks associated with ERCP, assisting you in deciding whether this procedure is fitting for your condition.
Key benefits of ERCP
- Quick symptom relief
ERCP can provide almost instant relief for patients suffering from intense abdominal pain, jaundice, nausea, vomiting, or indications of biliary infection caused by ductal obstructions or strictures. Often, the procedure averts the worsening of symptoms into serious systemic issues.
- Immediate therapeutic action
One of the most notable clinical benefits of ERCP is its capacity to deliver treatment concurrently with diagnosis. For patients facing ductal blockages, strictures, or leaks, this combined approach minimizes the necessity for multiple procedures and accelerates recovery. Therapeutic interventions performed during ERCP may include stone removal, stent insertion to alleviate blockages, sphincterotomy for regulating flow, sealing of bile leaks, and dilation of constricted ducts. This therapeutic function makes ERCP particularly valuable in managing acute or complex biliary and pancreatic cases.
- Mitigation of severe complications
By addressing obstructions or leaks promptly, ERCP significantly reduces the likelihood of bile duct infection, pancreatitis, liver impairment due to extended bile retention, biliary cirrhosis, and secondary complications associated with undiagnosed cancers. ERCP can also act as a precursor to surgery or cancer treatment when biopsy samples or stent placements are necessary before surgery.
- Decreased requirement for open surgery
In numerous instances, ERCP negates the need for invasive abdominal surgery. This is especially advantageous for older patients or those with comorbidities who may not be suitable candidates for surgery. Recovery periods are shorter, and the overall burden on patients is considerably lessened.
- Focused biopsy and oncological evaluation
In situations where biliary or pancreatic tumours are suspected, ERCP facilitates targeted brush cytology or biopsy collection. This allows for earlier and more precise identification of malignancies and aids in timely referrals for cancer treatment.
Risks and complications of ERCP
While ERCP is regarded as a safe procedure when conducted by skilled gastroenterologists, it does carry certain risks. Although the rates of complications are low, they are significant, particularly in patients with pre-existing health issues.
- Bleeding
Bleeding is more likely to happen after a sphincterotomy or in patients receiving anticoagulation therapy. The majority of post-ERCP bleeding cases are mild and can be managed endoscopically. Severe bleeding is uncommon and may necessitate transfusion or surgical intervention.
- Infection
Infection can arise if the bile ducts are not adequately drained after the procedure. This risk is heightened in patients with strictures or incomplete stone removal. Prophylactic antibiotics and post-procedure drainage are crucial preventive strategies.
- Perforation
Duodenal or ductal perforation is a rare but serious risk. Patients with altered anatomy or diverticula near the ampulla face an increased risk. Surgical repair may be necessary in these instances, although some perforations can be treated conservatively.
- Post-ERCP Pancreatitis
This is the most frequently encountered complication, occurring in about 3–10% of cases. In most situations, it is mild and self-resolving; however, moderate to severe pancreatitis may necessitate hospitalization, intravenous fluids, and careful monitoring. Risk factors include previous history of pancreatitis, sphincter of oddi dysfunction, and difficult cannulation during the procedure. Preventive measures such as rectal NSAIDs and prophylactic pancreatic stents are commonly employed in patients at high risk.
- Sedation-related complications
ERCP is typically performed under conscious sedation or general anaesthesia. As with any procedure involving sedation, complications such as respiratory depression or cardiac instability may arise, especially in elderly or high-risk patients. Proper pre-anaesthetic evaluation and monitoring during the procedure are vital.
- Allergic reactions
Reactions to contrast dye are rare, yet they can vary from mild symptoms such as rash and itching to severe cases like anaphylaxis. It is essential for patients with known iodine allergies to notify the healthcare team before undergoing the procedure.
Who should be cautious?
While ERCP can be life-saving or curative, certain patient groups necessitate a more thorough evaluation before proceeding:
- Those with a previous history of post-ERCP pancreatitis
- Patients with known allergies to contrast agents
- Individuals with complex surgical anatomy
- Elderly patients with cardiac or pulmonary comorbidities
- Individuals with coagulopathies or those on anticoagulant therapy
In these situations, the choice to move forward with ERCP should be informed by a comprehensive benefit-risk assessment, often supplemented by alternative diagnostic methods.
Is ERCP right for you?
The suitability of ERCP is contingent upon a variety of factors, including the urgency of your condition, available alternative diagnostic methods, and your individual risk profile. Typically, the procedure is advised when:
- Immediate therapeutic action (e.g., stone extraction or stenting) is required
- Biopsy or tissue sampling is essential for diagnostic precision
- Non-invasive imaging tests (MRI, CT, ultrasound) indicate obstructive or structural issues
- The potential risks are outweighed by the necessity for prompt symptom relief or prevention of complications
ERCP presents a highly effective, minimally invasive method for diagnosing and treating serious biliary and pancreatic disorders. Its capacity to deliver real-time therapeutic interventions renders it an essential tool in contemporary gastroenterology. Nevertheless, it is a complex procedure that must be undertaken with a clear comprehension of the associated risks. A comprehensive discussion with your gastroenterologist – backed by pre-procedural imaging, laboratory tests, and medical history – is vital in deciding whether ERCP is the appropriate option for you. When conducted by skilled professionals and with adequate precautions, the advantages of ERCP frequently surpass the risks, providing patients with both immediate relief and long-term clinical benefits.
If you’re considering ERCP in Ahmedabad, Mission Gastro Hospital is a trusted centre for advanced gastrointestinal care. With experienced gastroenterologists and state-of-the-art endoscopy facilities, the hospital ensures safe, effective, and patient-focused ERCP procedures. So, approach the hospital if you’re considering the procedure to learn if you are eligible for it, and to get the best assistance.