When discussing medical procedures like colonoscopy, many individuals believe it is a consistent experience for all – a standardized test performed identically regardless of gender. After all, both men and women possess colons, and the screening method itself is comparable. However, beneath this apparent uniformity exists a range of significant gender-specific distinctions. From hormonal factors and pregnancy considerations to the manifestation of symptoms and the progression of certain diseases, women’s digestive health, and their colonoscopy experience, can vary considerably from that of men. Recognizing these differences is not merely about being informed; it is about empowering women to approach colonoscopy with assurance, comfort, and the necessary knowledge to make educated healthcare choices.
Why colonoscopy matters for women
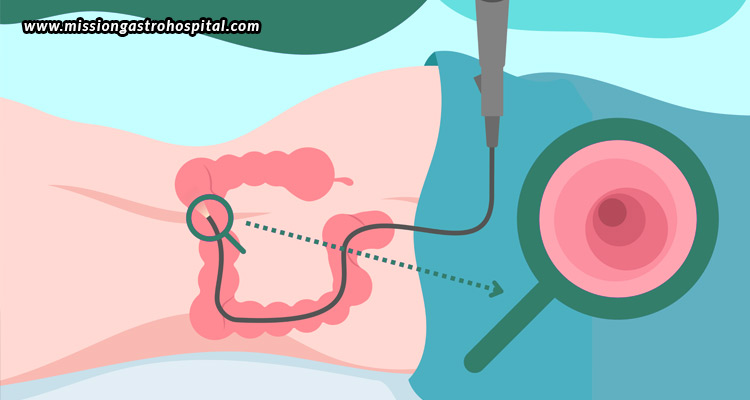
Colonoscopy serves as one of the most powerful methods for preventing colorectal cancer, which ranks as the third most prevalent cancer among women. This procedure enables gastroenterologists to directly examine the inner lining of the colon and rectum, identify precancerous polyps, and eliminate them before they can become cancerous. Nevertheless, research indicates that women are sometimes less inclined to receive timely colonoscopies compared to men, often due to misunderstandings, feelings of embarrassment, or the incorrect assumption that their risk is lower. In truth, women have a similar lifetime risk of developing colorectal cancer, and for some, this risk may increase due to specific hormonal or reproductive factors. Undergoing screening at the right time and with the right medical supervision is crucial. For women seeking expert care, Mission Gastro Hospital offers access to some of the best colonoscopy doctors in Ahmedabad, ensuring safe, accurate, and compassionate screening tailored to women’s unique health needs.
Hormonal effects on digestive health
The gastrointestinal systems of women are profoundly influenced by hormonal shifts throughout their lives – during menstruation, pregnancy, and menopause. These hormonal variations affect motility, sensitivity, and overall bowel function, which can impact both symptoms and the colonoscopy experience itself.
- Menstrual cycle and bowel function
Oestrogen and progesterone play a role in gastrointestinal motility. Many women experience changes in digestion during their menstrual cycle – such as bloating, constipation, or diarrhoea – which can affect their comfort level prior to a colonoscopy. For instance, scheduling a colonoscopy in the middle of the cycle may alleviate discomfort and cramping during the preparation phase.
- Pregnancy and colonoscopy
Colonoscopy is generally avoided during pregnancy unless absolutely necessary, such as in cases of severe gastrointestinal bleeding or flare-ups of inflammatory bowel disease. If a colonoscopy is required during pregnancy, it is usually performed in the second trimester when the risks are minimized. Adjustments include utilizing minimal or pregnancy-safe sedation, carefully positioning the patient to prevent pressure on the uterus, and ensuring close collaboration between the gastroenterologist and obstetrician. For women considering pregnancy, it is often advised to complete screening prior to conception, particularly if there is a family history of colorectal cancer or chronic bowel conditions.
- Menopause and beyond
The decline in hormones during menopause frequently leads to slower digestion and a heightened risk of constipation. Postmenopausal women also face an increased risk of colorectal cancer, especially if hormone replacement therapy (HRT) is not utilized. Conversely, research indicates that women who have undergone HRT may experience a slightly reduced risk of colorectal cancer, although this does not substitute for regular screening.
Understanding these hormonal influences at different life stages enables women to plan the timing of their colonoscopy more comfortably and effectively.
Anatomical and technical differences
Although the colon operates similarly in both men and women, there are certain anatomical differences that can lead to variations in the colonoscopy experience.
- Longer colon and loops
Typically, women possess a longer and more flexible colon compared to men. This additional length and mobility, particularly in the transverse colon, can complicate navigation during the procedure. Skilled gastroenterologists employ specific techniques and make equipment adjustments to reduce discomfort and guarantee thorough visualization.
- Pelvic anatomy and prior surgeries
Pelvic components such as the uterus and ovaries, along with past gynaecological surgeries (including C-sections or hysterectomies), can result in adhesions or anatomical differences that influence the movement of the colonoscope. This may sometimes cause mild discomfort or necessitate slightly extended procedure durations, but experienced specialists can modify their methods as needed.
- Differences in pain perception
Studies suggest that women may possess increased visceral sensitivity, which means they could feel discomfort more intensely than men during procedures involving internal organs. Therefore, effective sedation and clear communication with the healthcare team are essential for ensuring comfort and relaxation throughout the colonoscopy.
Colonoscopy and reproductive health
The reproductive milestones of women – including pregnancy, childbirth, and menopause – can significantly impact bowel habits and the necessity for screenings.
- Postpartum changes
After childbirth, hormonal fluctuations and temporary alterations in diet or physical activity can influence digestion. Women who notice rectal bleeding or changes in bowel habits following delivery should not automatically attribute it to haemorrhoids; a colonoscopy may be recommended if symptoms continue.
- Infertility evaluations
In certain cases, a colonoscopy is suggested prior to fertility treatments, particularly if there is a history of inflammatory bowel disease (IBD) or ongoing gastrointestinal symptoms, to rule out any underlying inflammatory or structural problems.
- Perimenopausal transition
Women nearing menopause might face issues like constipation and bloating due to hormonal shifts. Additionally, a colonoscopy can be scheduled alongside other midlife screenings, such as mammograms, as part of a comprehensive health strategy.
Screening recommendations for women by age
Although age-appropriate screening guidelines apply broadly, women may need different timelines due to unique hormonal and reproductive risk factors.
- Ages 20–39: Early awareness
Routine colonoscopy is generally not necessary unless there is a family history of colorectal cancer or inherited conditions such as Lynch syndrome. Nevertheless, any ongoing changes in bowel habits should be assessed. Women in this age group should also focus on maintaining gut health through a nutritious diet, sufficient hydration, and consistent physical activity.
- Ages 40–49: Early screening for high-risk individuals
If a first-degree relative was diagnosed with colorectal cancer before the age of 60, screening should commence at age 40 or ten years prior to the diagnosis of the affected relative. This is particularly crucial for women with family histories of breast, ovarian, or endometrial cancers, as these may suggest shared genetic risks.
- Ages 50 and above: Routine screening
For the majority of average-risk women, colonoscopy should begin at ages 45–50, based on national or institutional guidelines, and should be repeated every 10 years if no abnormalities are detected. For women with a history of polyps, inflammatory bowel disease, or a family history, shorter screening intervals (every 3–5 years) may be advised.
Colonoscopy is more than a medical procedure; it represents a proactive approach to managing your long-term health. Although the procedure is essentially the same for all individuals, women’s bodies – shaped by hormonal, anatomical, and life-stage factors – require particular attention. By understanding these differences, scheduling the procedure thoughtfully, and collaborating with a knowledgeable specialist, women can transform colonoscopy into a comfortable, enlightening, and potentially life-saving experience. Screening is not something to fear; it is a pathway to prevention, assurance, and enduring wellness.